
Will people with spinal hernias be drafted? What the Medical Examination Commission decides and when you can appeal the decision
The question of whether you can be mobilized with a spinal disc herniation does not have a universal “yes” or “no” answer. The mere presence of an intervertebral disc herniation does not automatically make a person unfit for military service, because for the Military Medical Commission (MMC/VLK) the key factor is not only the diagnosis but, first and foremost, how much the condition actually impairs body functions: whether there is a persistent pain syndrome, restricted mobility, neurological complications, post-surgical consequences, or other confirmed changes that affect fitness.
Will you be mobilized with a spinal disc herniation?
Yes, you can be mobilized with a spinal disc herniation. But not in every case. If the hernia does not cause significant or medically documented functional impairments, the MMC most often does not see grounds to declare unfitness. If there are pronounced functional impairments, the condition is assessed under Article 64 of the Schedule of Diseases, and in cases after acute conditions, exacerbations of chronic diseases, or surgical treatment, Article 65 on temporary unfitness may be applied.
So the key question is not “do you have a hernia,” but “what consequences does it cause and what evidence confirms it.” This is what the MMC’s conclusion is based on.
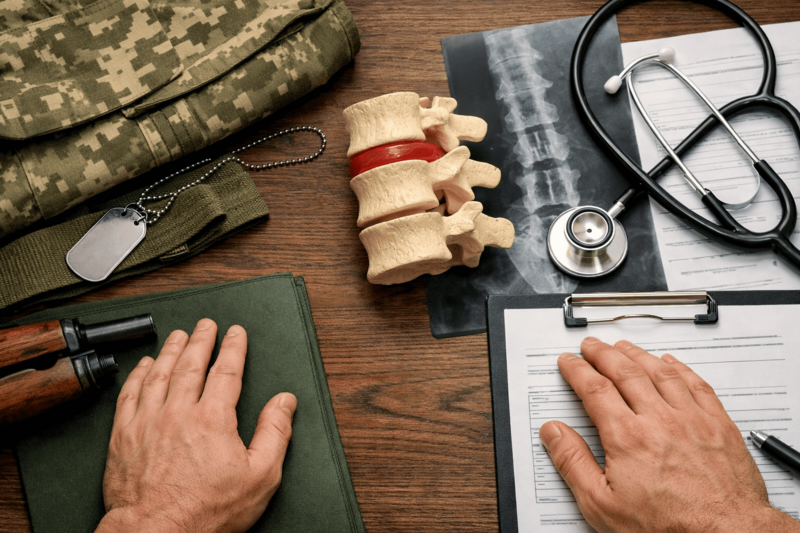
Which legal rules govern fitness decisions for spinal herniation
What Order of the Ministry of Defense of Ukraine No. 402 Is
The core document for military medical examination is Order of the Ministry of Defense of Ukraine No. 402 dated 14.08.2008, which approved the Regulation on Military Medical Examination in the Armed Forces of Ukraine. It is published in the database of the Verkhovna Rada of Ukraine as a valid act. This regulation sets out how the MMC operates, how conclusions are formulated, and includes the Schedule of Diseases used to assess fitness.
What Article 64 of the Schedule of Diseases provides
Article 64 of the Schedule of Diseases covers spinal disorders (dorsopathies) and their consequences under ICD-10 codes M40–M54, including kyphosis and lordosis, scoliosis, spinal osteochondrosis, spondylolysis, spondylolisthesis, intervertebral disc disorders, and other dorsopathies. An intervertebral disc herniation falls within the conditions assessed under this article. Article 64 provides the following framework: with significant functional impairments — unfit for military service; with moderate functional impairments — fit for service in designated support units, Territorial Centers for Recruitment and Social Support (TCRSS/TCC & SP), military higher education institutions, training centers, facilities (institutions), medical units, logistics, communications, operational support, and security units; with minor functional impairments or objective findings without functional impairment — fit.
Why the MMC assesses not only the diagnosis but functional impairment
The logic of Order No. 402 is built around assessing the degree of functional impairment. Therefore, the wording “disc herniation” alone is not enough. For the Commission, real clinical manifestations matter: restricted mobility, persistent pain, radiating pain, numbness, weakness, reduced reflexes, gait disturbance, need for surgery, frequent exacerbations, and the need for inpatient treatment. The MMC medical examination report must reflect anamnesis and objective findings, specialist examinations, and special test results.
When a spinal hernia may affect mobilization
An intervertebral hernia without significant functional impairments most often is not a basis for unfitness. If there are only MRI findings of a hernia but no stable functional disorders, the MMC usually treats the condition as minor impairment or objective findings without impairment. In that situation, a conclusion of unfitness is unlikely.
A different situation is a hernia with a pronounced pain syndrome that is not just a one-time complaint but is supported by medical records: repeated visits, courses of treatment, injections/blocks, recommendations to limit physical load. Pain also must be documented in doctors’ notes and medical records, not only “from the patient’s words.”
The MMC should assess even more carefully hernia cases with neurological complications: radicular syndrome, paresis, persistent numbness, reduced muscle strength, sensory loss, changes in reflexes, problems with mobility. Such states may indicate moderate or significant functional impairment depending on severity and persistence.
A separate category is the post-operative state after spine surgery. If a person has recently undergone surgery and is in treatment or rehabilitation, the issue may be considered not only under Article 64 but also under Article 65, which covers conditions after acute diseases, exacerbations of chronic diseases, and surgical treatment. Article 65 provides the conclusion “temporarily unfit; requires treatment, leave, or exemption from duties.”
Which spinal conditions and related diagnoses the MMC most often considers
Hernias and intervertebral disc disorders
Article 64 explicitly includes intervertebral disc disorders. This is where protrusions, extrusions, sequestered hernias, and chronic discogenic pathology usually fall if they affect function. The mere fact of sequestration also does not automatically mean unfitness, but it is a serious reason for a detailed assessment of consequences.
Scoliosis, kyphosis, lordosis, and other curvatures
The same article includes kyphosis, lordosis, and scoliosis. The MMC therefore assesses not only the hernia as a standalone diagnosis but the overall spinal pathology complex, especially when curvatures, degenerative changes, and disc pathology coexist.
Osteochondrosis, spondylolysis, spondylolisthesis
Osteochondrosis, spondylolysis, and spondylolisthesis are also explicitly listed in Article 64. In practice, this matters when the hernia is not the only issue but part of a chronic degenerative spinal process. In such cases the MMC should evaluate the combined impact of all changes on function, not isolate one diagnosis.
Trauma consequences and post-surgical states
If there are old spinal injuries, fracture consequences, implanted hardware, chronic post-surgical pain, or restricted mobility, all of this matters for the MMC. A post-operative state can be grounds for temporary unfitness during recovery, and later for assessing persistent functional impairment.
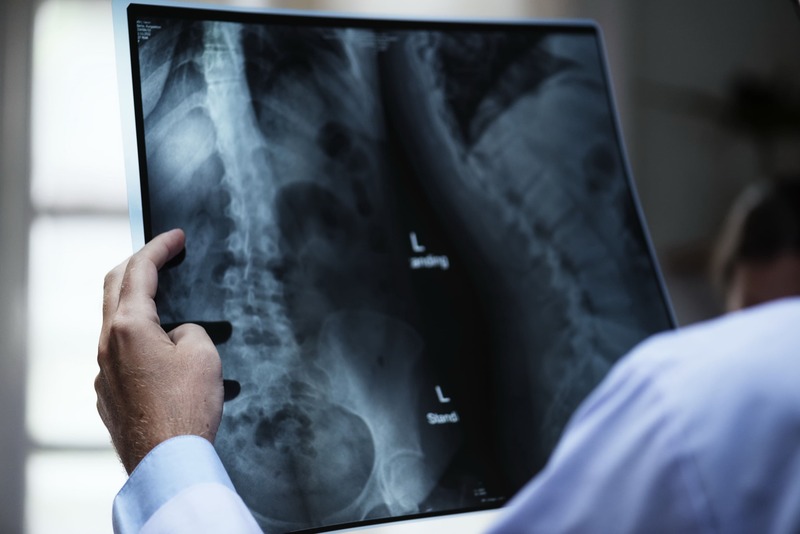
How the MMC determines fitness with a spinal hernia
The Commission evaluates symptoms and their persistence. Important factors include not only pain complaints but also restricted movement, inability to stand or walk for long periods, limited bending/extension, radicular symptoms, reduced muscle strength, numbness, sensory loss, exacerbations requiring treatment, and post-surgical consequences. The better this is supported by documents, the harder it is for the MMC to formally classify the case as “objective findings without functional impairment.”
Instrumental tests and specialist opinions are considered. Typically these include MRI, CT, X-ray, neurologist/orthopedist/neurosurgeon reports, hospital discharge summaries, information on medication therapy, physiotherapy, rehabilitation, nerve blocks, or surgery. The MMC assesses everything in combination, not based on a single document.
That is why the same diagnosis does not always lead to the same conclusion. For one person a hernia may be an incidental MRI finding; for another it may cause a persistent neurological deficit and constant flare-ups. For the MMC these are different cases.
What documents to prepare for the MMC for a spinal hernia
Before an MMC examination for a spinal hernia, it is advisable to prepare a complete set of medical documents. First of all, this includes up-to-date MRI, CT, or X-ray results, depending on the pathology. The most persuasive are usually imaging studies that clearly describe the hernia’s location, size, nerve root compression, and other complications.
Hospital discharges, outpatient records, notes of repeated visits, prescribed treatment and its outcomes are also important. If there were hospitalizations due to exacerbations, documents relevant to deferment on health grounds should be submitted as well.
Special value is given to neurologist/orthopedist/neurosurgeon conclusions that describe not only the diagnosis but functional impairments: pain, restricted movement, weakness, sensory disturbance, radicular syndrome, recommendations to limit physical load. If surgery was performed, provide operative reports, post-operative recommendations, and rehabilitation documents.
When a spinal hernia may lead to unfitness vs fitness
Unfitness under Article 64 is linked to significant functional impairments. This is not merely a hernia on imaging but a condition with pronounced and persistent functional limitations that are properly documented.
If impairments are considered moderate, Order No. 402 currently provides not full unfitness but fitness for service in designated support units, TCRSS/TCC & SP, training centers, medical, logistics, communications, and security units. This is important because many people rely on outdated approaches.
Fitness is most often concluded when there are minor impairments or only objective findings without proven functional disorders. That is why a person who reports pain verbally without systematic examinations and documented evidence is in a much weaker position before the MMC than someone with a properly documented medical history.
What to do if the MMC ignored your actual health condition
An MMC decision can be appealed. Regulation No. 402 provides that complaints against actions/inaction/decisions and conclusions of non-staff MMCs are filed to staff MMCs or to court; a regional MMC decision can be appealed to the Central MMC (CMMC/CVLK) or in court; and CMMC decisions can be appealed in court.
It makes sense to appeal when the Commission did not consider existing documents, failed to assess functional impairments, ignored post-surgical consequences, did not refer for additional examinations, or reduced a serious pathology to a formal diagnosis without clinical assessment. Under Order No. 402, when a complaint is substantiated, a staff MMC may review the conclusion or refer the person for a repeat/control medical examination.
The most common MMC mistakes in such cases are incomplete review of medical documents, no assessment of neurological signs, ignoring repeated exacerbations or a post-operative state, and a formal approach without additional testing. A military lawyer in such matters helps assemble the evidence, draft an appeal, tie medical documents to Articles 64 or 65, monitor the repeat examination procedure, and, if necessary, go to court.

Frequently asked questions
Can you be mobilized with an intervertebral hernia in Ukraine?
Yes. Everything depends on what functional impairments the hernia causes and how this is medically documented.
Does a spinal hernia automatically make you unfit for military service?
No. There is no automatic unfitness based on the diagnosis alone. The MMC assesses the degree of functional impairment.
Which article of Order No. 402 applies to a spinal hernia?
Most often, Article 64 of the Schedule of Diseases, which covers dorsopathies and intervertebral disc disorders.
Can you be mobilized with a sequestered hernia?
You can, if there are no proven significant functional impairments. However, a sequestered hernia requires especially careful assessment, particularly if neurological complications are present.
Can you be mobilized after surgery to remove a spinal hernia?
It depends on the recovery stage and the consequences of surgery. During treatment or rehabilitation, Article 65 (temporary unfitness) may apply, and later the assessment under Article 64 depends on persistent functional impairments.
Can an MMC decision be appealed in a spinal hernia case?
Yes. First — to a higher MMC within the chain of authority, and in certain cases — to the Central MMC or to court.
Do you need a lawyer to appeal an MMC decision?
The law does not require the mandatory involvement of a lawyer. In practice, however, legal help is useful when you need to correctly align medical documents with the relevant article of the Schedule of Diseases and prepare a procedurally strong complaint or claim.
Conclusion
A spinal hernia does not mean automatic unfitness for mobilization. What matters is what the MMC can see and confirm: how pronounced the functional impairments are, whether there are neurological complications, whether treatment was carried out, whether there were surgeries, exacerbations, and limitations in everyday life. If the Commission ignored the real health condition or handled the case formally, the conclusion can and should be appealed in the established manner. Careful legal and medical preparation in such cases often matters no less than the diagnosis itself.
Leave a request for consultation and our specialist will contact you soon!
Leave a request and our specialist will contact you soon!
More useful information
Fill out the form or contact us in any way convenient for you
Choose the nearest office to you and receive consultations in a convenient format for you




